The unspoken problem with California nursing homes is staffing. Not enough of it, and poor training for those who do it. Who knows what caused this major screw up, but you can be sure it’s related to staffing. A 94-year-old resident of Silverwood Senior Living Facility, a skilled nursing facility, went missing last month. Staff searched everywhere for the dementia patient, but couldn’t find her.
Thankfully, someone thought to check the walk-in freezer in the nursing home kitchen. There they found the resident locked inside the freezer where the temperature was set at five degrees. Thankfully she was unharmed. Still no one knows just how she got in the freezer, and the home, who has a history of regulatory violations, self-reported the incident as required by law.
Mark Mostow, a VP for the nursing home, released this obligatory statement about the resident: “We immediately conducted an investigation, and took appropriate corrective action against two employees. It’s an unfortunate incident, and we’re very sorry that it happened, and we’ll do everything in our power to ensure this does not happen again.”
 California Nursing Home Abuse Lawyer Blog
California Nursing Home Abuse Lawyer Blog


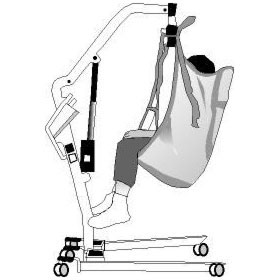 An investigation by the Department of Public Health revealed that the nursing home, the Eskaton Care Center, failed to properly maintain the lift. The lift, which law required be checked monthly, had not been checked for five years. The DPH report stated that the sling appeared worn and had “what appeared to be bleached out blood stains at the center.”
An investigation by the Department of Public Health revealed that the nursing home, the Eskaton Care Center, failed to properly maintain the lift. The lift, which law required be checked monthly, had not been checked for five years. The DPH report stated that the sling appeared worn and had “what appeared to be bleached out blood stains at the center.” The
The 





