Articles Posted in California Department of Public Health
Was it Nursing Home Negligence or Neglect? Does it matter?
 When we place a loved one in a nursing home or assisted living facility, we are placing enormous trust in that facility’s staff. We trust them to provide not just basic care, but dignity, safety, and attention.
When we place a loved one in a nursing home or assisted living facility, we are placing enormous trust in that facility’s staff. We trust them to provide not just basic care, but dignity, safety, and attention.
So when something feels wrong—unexplained injuries, sudden decline, dehydration, infections, or emotional withdrawal—it is natural to feel alarmed. Many families ask the same question:
Is this negligence or neglect?
Can I Sue a Nursing Home in California for Bed Sores?
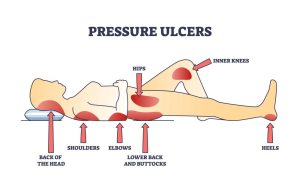 When a loved one develops a large, painful bed sore in a nursing home, it is almost always a sign that something went terribly wrong. Families often feel a mix of anger, guilt, and confusion — and they want to know one thing: Can I sue a nursing home in California for allowing this to happen? The answer is yes. Under California law, bed sores are a preventable medical condition, and when they occur, they often indicate neglect.
When a loved one develops a large, painful bed sore in a nursing home, it is almost always a sign that something went terribly wrong. Families often feel a mix of anger, guilt, and confusion — and they want to know one thing: Can I sue a nursing home in California for allowing this to happen? The answer is yes. Under California law, bed sores are a preventable medical condition, and when they occur, they often indicate neglect.
Below is a clear, compassionate explanation of your rights and what to do next.
What a Bed Sore Really Means in a Nursing Home
Nursing Home Residents Have the Right to Leave: Understanding California Law
 Is there any right more fundamental than the freedom to leave a place where you do not wish to stay? For nursing home residents in California, this right is often disregarded—sometimes in direct violation of the law. Fortunately, the California Advocates for Nursing Home Reform (CANHR) has recently updated its guide for long-term care residents who are being held against their will. This guide outlines the legal protections available and provides practical steps to challenge illegal restrictions on a resident’s right to leave.
Is there any right more fundamental than the freedom to leave a place where you do not wish to stay? For nursing home residents in California, this right is often disregarded—sometimes in direct violation of the law. Fortunately, the California Advocates for Nursing Home Reform (CANHR) has recently updated its guide for long-term care residents who are being held against their will. This guide outlines the legal protections available and provides practical steps to challenge illegal restrictions on a resident’s right to leave.
The Right to Move Freely
Imagine you live independently in an apartment, making your own choices and living life on your own terms. One day, your landlord locks you inside, installs alarms on your doors and windows, and tells you that you’re not allowed to leave. He insists that, for your own safety, you must remain inside indefinitely. When you call the police for help, they tell you that your situation is a “civil matter” and that you need a court order to be able to leave.
Why Nursing Home Offenses in Los Angeles County May Not be Reported to the Public
When families in Los Angeles County or elsewhere in Southern California are seeking information about nursing homes and skilled nursing facilities in the state, they often turn to the CMS star rating system and to publicly available information about safety violations. Yet according to a recent report in The New York Times, some of the worst offenses at nursing homes across the country might not be reported to the public. Why are serious nursing home abuse and neglect injuries hidden? The report suggests that a “secretive appeals process” prevents the public from getting the full picture. Our Los Angeles County nursing home abuse attorneys can tell you more.
Serious Injuries are Not Factored Into the Star Rating System
The Centers for Medicare and Medicaid Services (CMS) publishes information about nursing homes through its star rating system, which is supposed to provide the public with information about recent safety violations at nursing homes and harms suffered by elderly residents. Yet the recent report, which stems from a New York Times investigation, indicates that “at least 2,700 . . . dangerous incidents were not factored into the rating system.”
CANHR Holding Town Hall on The Current State of Visitation Rights
 The California Advocates for Nursing Home Reform (CANHR) is a statewide nonprofit that has been dedicated to improving the choices, care and quality of life for California’s nursing home residents and families.
The California Advocates for Nursing Home Reform (CANHR) is a statewide nonprofit that has been dedicated to improving the choices, care and quality of life for California’s nursing home residents and families.
On Jul 21, 2021 at 12:00 pm, CANHR will be holding an online town hall to discuss nursing home visitation rights in the Covid era. The goal of the town hall is to provide information to participants about the current state of the statewide visitation rules, and explain how advocacy can be used to gain more visitation access. There will also be a Q&A.
The town hall speakers will be CANHR staff attorneys Tony Chicotel and Mike Dark and Essential Caregivers Coalition co-founders Maitely Weismann and Melody Taylor Stark.
California Nursing Home Inspections Slated to Restart
Over the last year during the COVID-19 pandemic, nursing homes in Los Angeles County and throughout Southern California were not subject to annual inspections by the California Department of Public Health because of the coronavirus lockdowns. In the last year, many commentators have worried that nursing home conditions—many of which were already poor—were likely to worsen given that friends and family members were not permitted to see nursing home residents and to be in a position to report signs of nursing home abuse and neglect, and that the California Department of Public Health would not be conducting inspections.
Whether those concerns ultimately prove to be a reality may become clearer in the coming weeks and months as the California Department of Public Health resumes its annual inspections of nursing homes in the state, according to a recent report from KPBS.
State Will Resume Annual Nursing Home Inspections
Obtaining Consent for Covid-19 Vaccinations from Elderly Nursing Home Residents
California received its first batch of Covid-19 vaccinations and began vaccinating people according to recommendations from the California Department of Health. First, the vaccine is being given to health care workers and residents of skilled nursing facilities, assisted living facilities and similar facilities for older and medically vulnerable patients.
 Currently, there are more than 400,000 people living in skilled nursing facilities (nursing homes, rehabilitation centers, convalescent hospitals) in California. Questions arise over how to obtain consent for the vaccines for the elderly who suffer from dementia or Alzheimer’s or in some other way lack the capacity to give consent. Obtaining written consent from the patient him or herself would be the best, but that is not going to be possible for many residents of nursing home and assisted living facilities.
Currently, there are more than 400,000 people living in skilled nursing facilities (nursing homes, rehabilitation centers, convalescent hospitals) in California. Questions arise over how to obtain consent for the vaccines for the elderly who suffer from dementia or Alzheimer’s or in some other way lack the capacity to give consent. Obtaining written consent from the patient him or herself would be the best, but that is not going to be possible for many residents of nursing home and assisted living facilities.
People are worried about the safety of vaccines, and some discount the severity of the virus itself. The federal government has not provided clear direction on how to best encourage people to consent to taking the vaccine. It is easy to imagine that within families there might be disagreement over whether a loved one should be vaccinated in the first place. These disagreements will need to be worked out because there is an urgent need to vaccinate the elderly who are disproportionately affected by Covid 19 and require hospitalization at higher rates than the rest of the population when they do get infected.
AA Citation Issued for Los Angeles County Nursing Home
Lomita Post-Acute Care Center of Los Angeles County, California was issued a Class AA Citation by the California Department of Public Health (CDPH) on August 14, 2020 after a resident was killed due to sepsis resulting from negligent patient care at the facility.
The Care Center failed to follow its own policies and procedures to ensure that the resident, who had been admitted just 7 days prior, received the care she needed, which started with an accurate assessment of the resident’s change of condition, in combination with urinary catheter care, reporting to the physician the resident’s change of condition in a timely manner, and sending the resident to the hospital only after a family member insisted.
Interviews and Nurses Notes indicated that on several instances there was no documented confirmation that the Resident’s catheter was being examined per physician’s orders. Which likely contributed to the UTI that later caused Sepsis in the Resident.
Compton Nursing Home Issued AA Citation in Nursing Home Fall Case
Santa Fe Heights nursing home in Compton was issued an AA citation by the California Department of Public Health (CDPH) on October 16, 2020 after a resident was seriously was killed in a fall that went unnoticed by staff.
The injured resident had four falls in four consecutive months despite being assessed by nursing home staff at being at high risk for falling. After the fourth fall, the resident was found on the floor unresponsive and without vital signs. An investigation by CDPH revealed that Santa Fe Heights failed to implement safety measure and provide adequate supervision to the resident and failed to develop a plan of care to address his growing fall risk.
Nursing notes revealed that at the time of the last (and fatal) fall, the resident was found by a CNA on the floor at 2:45 pm after attempting to transfer from the toilet. He reportedly hit his head in the fall and was promptly returned to bed without a neuro-check being performed. Despite his obvious signs of injury, including a laceration on his head, there was no assessment for injury, nor any follow up.
 California Nursing Home Abuse Lawyer Blog
California Nursing Home Abuse Lawyer Blog









