 Yes. If your loved one developed bed sores while living in a nursing home or assisted living facility in Riverside County, you may have the right to file a lawsuit for neglect. Pressure sores are widely recognized as a preventable condition when residents receive proper care and supervision. When a facility allows these wounds to develop or worsen, it often signals serious failures in basic caregiving. A qualified Riverside bed sore lawyer can investigate whether neglect contributed to the injury and help your family pursue accountability.
Yes. If your loved one developed bed sores while living in a nursing home or assisted living facility in Riverside County, you may have the right to file a lawsuit for neglect. Pressure sores are widely recognized as a preventable condition when residents receive proper care and supervision. When a facility allows these wounds to develop or worsen, it often signals serious failures in basic caregiving. A qualified Riverside bed sore lawyer can investigate whether neglect contributed to the injury and help your family pursue accountability.
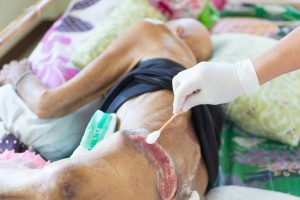
How Bed Sores and Pressure Wounds Develop
Bed sores, also known as pressure ulcers or pressure injuries, form when prolonged pressure on the skin cuts off blood flow to the tissue underneath. This most commonly occurs in elderly residents who cannot reposition themselves without assistance.
 California Nursing Home Abuse Lawyer Blog
California Nursing Home Abuse Lawyer Blog










